Why Foot Wounds Are Problematic for Diabetics
Millions of people in America suffer from diabetes, which often leads to complications in their feet. Diabetes impairs the body’s ability to regulate blood glucose levels. This, in turn, disrupts the functionality of white blood cells which are critical in closing wounds. Additionally, diabetes can lead to poor circulation, and this reduces the amount of nutrients sent to wound sites and further impairs the healing process. Neuropathy, or nerve damage, is another condition associated with diabetes. Neuropathy further complicates diabetic wound management because it can prevent diabetic adults from feeling when there is trauma or an injury to their skin, and wounds may progress before they are even discovered. All of these factors combined make the diabetic wound harder to detect and heal, which may lead to infection and worse—if it's not treated properly. If you are diabetic, it's important to be under the care of a podiatrist who can offer preventative measures against foot wounds and treat them promptly and properly if they do develop.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Edward S. Pozarny DPM from Arlington Podiatry Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Arlington, VA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
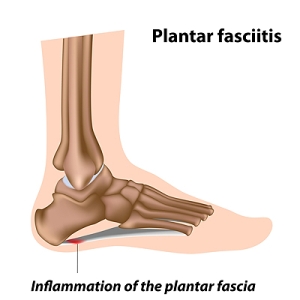
What Causes Plantar Fasciitis?
 The plantar fascia is the band of tissue that run along the bottom of the foot and connects the heel to the toes. When the plantar fascia becomes inflamed or partially torn, it results in the condition that is commonly referred to as plantar fasciitis. Plantar fasciitis is one of the most common causes of heel pain. The pain is usually worse in the morning and after long periods of rest. Common causes of plantar fasciitis includes sitting or standing for long periods of time, having tight calf muscles, having flat feet or high arches, obesity, and arthritis. Patients who are struggling with heel pain should consult with a podiatrist because there are a variety of causes. Once you visit with a podiatrist, they will be able to provide a proper diagnosis, as well as a customized treatment plan for your condition.
The plantar fascia is the band of tissue that run along the bottom of the foot and connects the heel to the toes. When the plantar fascia becomes inflamed or partially torn, it results in the condition that is commonly referred to as plantar fasciitis. Plantar fasciitis is one of the most common causes of heel pain. The pain is usually worse in the morning and after long periods of rest. Common causes of plantar fasciitis includes sitting or standing for long periods of time, having tight calf muscles, having flat feet or high arches, obesity, and arthritis. Patients who are struggling with heel pain should consult with a podiatrist because there are a variety of causes. Once you visit with a podiatrist, they will be able to provide a proper diagnosis, as well as a customized treatment plan for your condition.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Edward S. Pozarny DPM from Arlington Podiatry Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Arlington, VA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
What Could Be Causing Pain in My Heel?
Heel pain is one of the most common reasons why people seek the care of a podiatrist. There are a number of conditions that trigger heel pain, with the leading cause being plantar fasciitis. This is a condition in which the plantar fascia—the long band of connective tissue spanning the bottom of the foot from heel to toe—becomes inflamed and painful from overuse, improper footwear, or other factors. Pain in the back of the heel, where the Achilles tendon attaches to the heel bone, is typically due to overuse and repetitive strain. When the fat pads that cushion the heel bone thin down with age (fat pad atrophy) pain can be felt in the heel. A painful bump or redness at the back of your heel are symptoms of Haglund’s deformity. This condition occurs when a bony enlargement causes inflammation in the soft tissue and bursa sac near the Achilles tendon. Psoriatic arthritis can cause inflammation, stiffness, and pain in joints where tendons and ligaments connect with bones, such as the heel. Heel pain may even be a symptom of heel spurs. If you experience any pain, stiffness, or other discomfort in your heel, make an appointment with a podiatrist who can diagnose and treat your condition.
Many people suffer from bouts of heel pain. For more information, contact Edward S. Pozarny DPM of Arlington Podiatry Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Arlington, VA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
Corns: What Are They, and How Do You Get Rid of Them
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much smaller than calluses.
Removing the dead skin that has built up is the key in treating corns. Salicylic acid medication is most common in accomplishing this. The acid works by dissolving keratin, which is the protein that makes up the majority of corns. You can purchase salicylic acid over-the-counter in products such as wart removers. It comes in a variety of forms such as medicated pads, drops, or creams. However, people who are diabetic should not use salicylic acid, but should instead consult their doctor immediately.
According to the product directions, applying the medication directly onto the corn will treat it. The top layer of the corn will begin to turn white after use. When that occurs, the layers of skin can then be peeled away, making the corn smaller. Shaving off corns with razors or other pedicure equipment is never a good idea. This can lead to infection. If your corn gets infected, and is not treated immediately, a visit to the doctor will be necessary.
Another way to treat corns and help prevent their return is by using orthotic inserts, fitted by a podiatrist. Inserts fit right into your shoes and adjusts the way your foot fits into your shoes. This fixes the way you walk. This will lower your chances of getting corns, and eliminate current corns by reducing rubbing from friction.
Surgery is rarely used to treat corns, but does occur on occasion. Surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub your feet. Pads can be purchased if you notice rubbing developing. These pads can be purchased over-the-counter, and can be simply placed on the irritated area. Wearing cushioned insoles in your shoes can always reduce the friction, and making sure to wear well-fitting shoes. This will ensure that your foot is not being squeezed awkwardly, and prevent corns from forming in the first place.
Helpful Tips for Measuring Your Feet
Planning a trip to the shoe store? Be sure to start with an accurate measurement to ensure you get shoes that are the right size. Start at the end of the day when your feet are at their largest, and stand up straight with one foot on a piece of paper (tape two pieces together if necessary). Carefully trace your foot’s shape with a pen or pencil held at a 90 degree angle. For the length: use a ruler or measuring tape to measure the tracing from the length of your foot from the bottom of your heel to the tip of the longest toe. To measure the width of your foot, wrap a measuring tape around the widest part of your foot (be sure you are pressing down the full weight of your body as you do it). Repeat the entire measuring process on your other foot. Check the largest measurements you’ve recorded against an online shoe size measurement tool to determine your ideal shoe size (length) and width (regular, wide, or extra wide). For more tips on choosing shoes most appropriate for your particular foot size and shape, consult with a podiatrist.
Getting the right shoe size is an important part of proper foot health. Seek the assistance of Edward S. Pozarny DPM from Arlington Podiatry Center. Our doctor will provide the care you need to keep you pain-free and on your feet.
Getting the Right Shoe Size
There are many people who wear shoes that are the incorrect size, negatively affecting their feet and posture. Selecting the right shoes is not a difficult process, so long as you keep several things in mind when it comes to choosing the right pair.
- When visiting the shoe store, use the tools available to measure your foot.
- Be sure there is ‘wiggle room’. There should be about an inch between your toes and the tip of your shoes.
- Do not always assume you are the same size, as manufacturers run differently.
- Purchase shoes later in the day, as your feet swell as the day progresses.
- If a shoe is not comfortable, it is not suitable. Most shoes can’t be ‘broken in’, and comfort should be the ultimate goal when it comes to choosing the right pair of shoes
As our feet hold our body weight and keep us moving, it is important to treat them right. Picking the right pair of shoes can provide your feet comfort and mobility without pain.
If you have any questions, please feel free to contact our office located in Arlington, VA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Getting the Right Shoe Size: To Keep Your Feet Happy
People are constantly wearing improperly-fitting shoes. Though it isn’t hard, picking the right shoes does require keeping a few things in mind.
Shoe stores have rulers so you can get an exact measurement of your feet. Be sure to always measure your feet with your shoes on. Measuring just your foot will give you a shoe size that is 1-2 inches too small for picking the right size shoe.
To ensure that your toes won’t be cramped, make sure there is wiggle room. Approximately one inch should be between your toes and the tip of your shoe. It is easy to tell if your shoes are too tight, because you will start to experience pain, blisters, and swelling.
Additionally, do not always assume your shoe size will be the same at every store. Manufacturers sometimes run differently, and your size will vary from brand to brand. Make sure the stores you purchase from have return policies, in case there is a problem.
Rather than shoe shopping in the morning, it is advised to shop for shoes later in the day. Your feet will swell as the day passes. If shoes are purchased in the morning, they may not be as snug as they should be. Furthermore, not all two feet are the same size. Therefore, accommodations may be necessary.
An overall concern in buying shoes is making sure they are comfortable and supportive. There is no such thing as a shoe being ‘broken in’. If they are uncomfortable at the store, they likely will always be uncomfortable.
Since we do a lot of walking, it is important that we pick the right shoes. Our feet will benefit from this, and we will be happier and healthier because of it.
A Toe Stretch for Plantar Fasciitis
 The plantar fascia is a ligament that runs along the bottom of the foot, and can be at risk of injury. When it is inflamed, usually due to repetitive overuse from playing sports or working out, plantar fasciitis may develop. Symptoms of this condition can include heel pain, arch pain, and possible swelling and tenderness along the bottom of the foot. There are many foot exercises that you can try to help relieve pain. Stretching is one way to help yourself recover from plantar fasciitis. One such exercise is the toe stretch. To do this exercise, sit on the floor with your knee bent and foot flat on the floor. Pull the toes back until you feel a stretch in the arch of your foot. Hold for 30 seconds, and then relax. Repeat 10 times. For more information about plantar fasciitis and foot stretches, please consult with a podiatrist.
The plantar fascia is a ligament that runs along the bottom of the foot, and can be at risk of injury. When it is inflamed, usually due to repetitive overuse from playing sports or working out, plantar fasciitis may develop. Symptoms of this condition can include heel pain, arch pain, and possible swelling and tenderness along the bottom of the foot. There are many foot exercises that you can try to help relieve pain. Stretching is one way to help yourself recover from plantar fasciitis. One such exercise is the toe stretch. To do this exercise, sit on the floor with your knee bent and foot flat on the floor. Pull the toes back until you feel a stretch in the arch of your foot. Hold for 30 seconds, and then relax. Repeat 10 times. For more information about plantar fasciitis and foot stretches, please consult with a podiatrist.
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with Edward S. Pozarny DPM from Arlington Podiatry Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
- Using a foam roller or any cylindrical object (a water bottle or soda can will do), roll the object under your foot back and forth. You should also exert pressure on the object. Be sure to do this to both feet for a minute. Do this exercise three times each.
- Similar to the previous one, take a ball, such as a tennis ball, and roll it under your foot while seated and exert pressure on it.
- Grab a resistance band or towel and take a seat. If you are using a towel, fold it length wise. Next put either one between the ball of your foot and heel and pull with both hands on each side towards you. Hold this for 15 seconds and then switch feet. Do this three times for each foot.
- Finally hold your big toe while crossing one leg over the other. Pull the toe towards you and hold for 15 seconds. Once again do this three times per foot.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising and ice and rest the foot. It is advised to then see a podiatrist for help.
If you have any questions, please feel free to contact our office located in Arlington, VA . We offer the newest diagnostic and treatment technologies for all your foot care needs.